Basal cell carcinoma (BCC) is the most common form of skin cancer, accounting for the majority of skin cancer diagnoses worldwide. It most frequently appears on sun-exposed areas, particularly the face.
While it is rarely life-threatening, it is locally invasive, meaning it can grow deeper into surrounding tissue if left untreated, making early detection essential.
For many patients, what begins as a small, subtle change can be an early sign of something more significant. Dr Derrick Phillips outlines what BCC cancer is, how to identify early stages of basal cell carcinoma skin cancer, and what treatment entails.
What Is Basal Cell Carcinoma (BCC)?
Basal cell carcinomas are named because the tumour cells resemble the basal cells found at the bottom of the epidermis. However, they are now thought to arise from cells within the hair follicle rather than directly from the surface layer of the skin.
Ultraviolet radiation plays a central role. Over time, cumulative UV exposure damages DNA within these cells, disrupting normal growth control. Instead of following the usual cycle of renewal and shedding, the cells begin to divide in an uncontrolled way, forming a slow-growing tumour.
What distinguishes basal cell carcinoma from other skin cancers is its behaviour. It very rarely spreads to distant organs, but it is not benign. These tumours can be locally invasive, gradually extending into surrounding tissue, including cartilage, bone and, in some cases, nerves.
This is why early treatment is important. Lesions on the face, particularly the nose and ears, are of particular concern, where anatomical structures are close to the surface and achieving clear surgical margins can be more challenging.
What Are the Early Signs of Basal Cell Carcinoma?
In its early stages, basal cell carcinoma can be subtle and is often mistaken for a minor skin concern.
Dr Phillips outlines 3 early stage signs to look out for:
- A spot that hasn’t healed and has persisted for months
- It has a pearly appearance and gradually grows
- Bleeding without touching it
Typical early features include a small, shiny or pearly bump, a flat red or pink patch, or a sore that does not heal. Some lesions may crust, bleed intermittently, or appear to heal and then recur. Others may resemble a scar-like area that feels firm or slightly waxy.
Because these changes can develop gradually, they are often dismissed. However, persistence is a key warning sign, particularly for any lesion that does not resolve over several weeks.
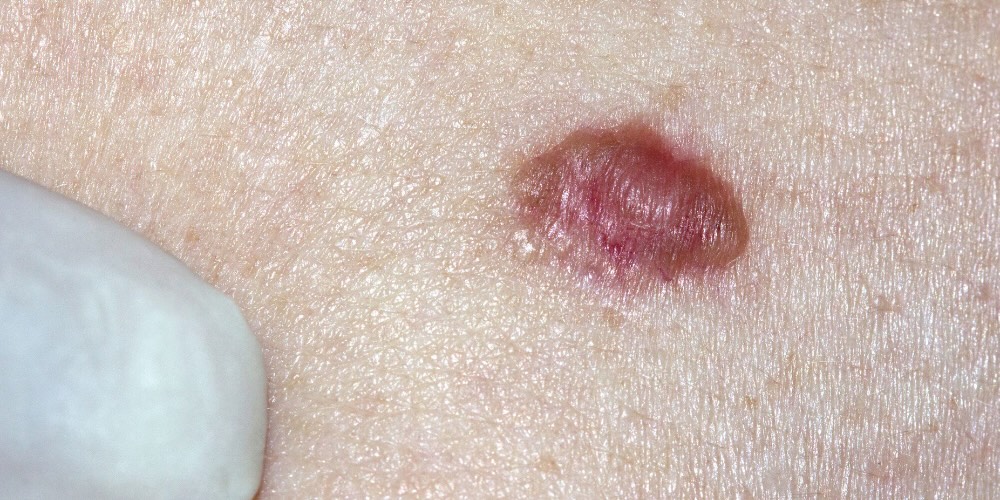
Basal Cell Carcinoma on the Face
Basal cell carcinoma is most common on the face because it is the area with the greatest lifetime sun exposure. The nose is the single most frequently affected site, followed by the cheeks, forehead, temples, and ears. Typically in areas where skin is thin, sun exposure is cumulative, and lesions can go unnoticed for months.
Because it can resemble a persistent pimple, a minor blemish, or a patch of dry skin, facial BCC is frequently dismissed in its early stages.
This matters because the face presents unique surgical challenges. Structures such as the nose, eyelids, and lips have limited surrounding tissue, which means that the deeper a lesion grows before treatment, the more complex the procedure required to remove it, and the greater the impact on cosmetic outcome. When identified early, treatment is typically straightforward and results are excellent. When delayed, the same lesion may require Mohs micrographic surgery or reconstructive work to achieve a clean margin.
If you notice any lesion on your face that is new, changing, bleeding without cause, or simply not healing, it warrants assessment by a dermatologist — regardless of how minor it appears.
Dr Derrick Phillips outlines what harmful skin changes to look out for in this video.
Can Basal Cell Carcinoma Appear on Other Parts of the Body?
Although basal cell carcinoma is most commonly associated with sun-exposed areas, it can occur anywhere on the body.
In addition to the face, BCC cancer may develop on the chest, back, shoulders, arms, and legs. In rarer cases, it can appear in areas with minimal sun exposure.
When lesions develop outside typical sun-exposed regions, other contributing factors may be involved, including previous radiotherapy, immunosuppression, or genetic predisposition.
Because basal cell carcinoma does not always follow predictable patterns, it is important to monitor any new, changing, or non-healing lesion anywhere on the body, not just areas exposed to the sun.
What Does Basal Cell Carcinoma Look Like on Black and Brown Skin?
Basal cell carcinoma is the most common form of cancer worldwide, but it predominantly affects fair-skinned populations due to cumulative UV exposure.
In individuals with black and brown skin, higher levels of melanin provide a degree of natural protection against UV radiation. As a result, basal cell carcinoma is less common in skin of colour, but it can still occur.
When present, it is often associated with specific risk factors such as immunosuppressive medications, genetic conditions, prior radiotherapy, or exposure to environmental carcinogens such as arsenic.
Importantly, the appearance of basal cell carcinoma in darker skin tones can differ from the classic presentation. Instead of a pink or pearly lesion, it may present as a dark brown or black, shiny or pearly growth. These lesions may bleed without provocation and can be mistaken for moles or melanoma.
This variation in presentation can lead to delayed diagnosis. For this reason, any lesion that changes, bleeds, or fails to heal should be assessed by a dermatologist, regardless of skin tone.
What Causes Basal Cell Carcinoma?
The primary cause of basal cell carcinoma is long-term exposure to ultraviolet (UV) radiation, which damages the DNA of skin cells.
Over time, this damage accumulates and can lead to uncontrolled cell growth. Risk factors include:
- Chronic sun exposure
- History of sunburns
- Use of tanning beds
- Fair skin, light eyes, or light hair
- Increasing age
While UV exposure is the dominant cause, other contributing factors such as immune suppression or prior radiation exposure can also play a role.
Basal Cell Carcinoma Treatment in the UK
Treatment is highly effective and depends on the size, location, and stage of the lesion.
Surgical removal is the gold standard, which may involve a standard excision or Mohs micrographic surgery, particularly for facial lesions where preserving healthy tissue is important.
For smaller or superficial lesions, non-surgical treatments may be appropriate. These include topical therapies, cryotherapy, or curettage and cauterization.
In more advanced or complex cases, additional therapies such as targeted medications or radiotherapy may be considered.
When treated early, outcomes are excellent, with a very high cure rate.
Basal Cell Carcinoma vs Other Skin Conditions: How to Tell the Difference
Because basal cell carcinoma can look like several common, benign skin concerns, it is frequently dismissed or misdiagnosed in its early stages. Understanding how it differs from other conditions can help you recognise when a lesion warrants professional assessment.
Dr Derrick Phillips outlines what bumps to look out for in this video.
Basal Cell Carcinoma vs Melanoma
Melanoma and basal cell carcinoma are both forms of skin cancer, but they behave very differently. Melanoma originates in the pigment-producing cells of the skin and is significantly more aggressive. It can spread to other organs if not caught early.
BCC, by contrast, grows slowly and rarely metastasises. In appearance, melanoma often presents as a dark, irregularly shaped lesion with uneven borders and multiple colours, while BCC is more commonly pearly, skin-coloured, or pink, and tends to be more uniform in appearance.
In darker skin tones, however, BCC can present as a dark brown or black shiny growth, which can make it harder to distinguish from melanoma without a dermatologist assessment. Any pigmented lesion that is new, changing, or bleeding should be evaluated promptly regardless of which it appears to be.
Dr Derrick Phillips outlines how to check your moles in this video.
Basal Cell Carcinoma vs Eczema
Eczema typically presents as red, itchy, dry patches that fluctuate with triggers such as stress, allergens, or changes in temperature. BCC does not itch in the same way and does not respond to moisturisers or topical steroids. A key distinguishing feature is persistence and behaviour over time. Eczema tends to come and go, while a BCC lesion will remain, slowly enlarge, and may bleed or crust without resolving. If a patch of skin that resembles eczema does not respond to standard treatment within a reasonable period, it should be assessed by a dermatologist.
Basal Cell Carcinoma vs a Pimple or Cyst
On the face, BCC is most commonly confused with a persistent pimple, or ingrown hair. The critical difference is that a pimple or minor blemish will resolve within days to weeks. A basal cell carcinoma will not. It may appear to improve briefly, but it will return, slowly grow, and may begin to bleed intermittently or develop a crusted surface. Any spot on the face that has been present for more than four to six weeks without resolving, particularly one that bleeds without being squeezed, should be examined.
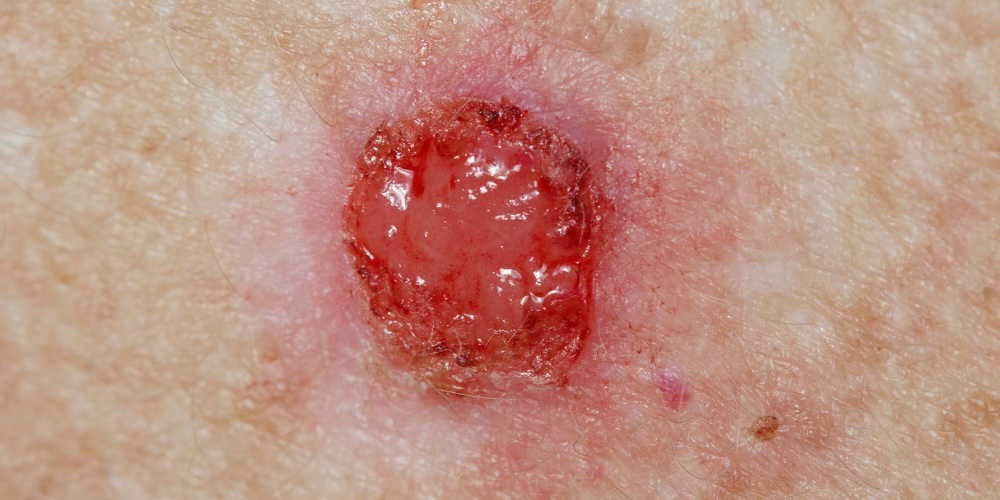
Basal Cell Carcinoma vs a Scar
Some subtypes of BCC, particularly morphoeic basal cell carcinoma, present as a flat, pale, scar-like area with slightly irregular edges. This is one of the most commonly missed presentations because it does not look like a typical skin cancer lesion. If you notice a scar-like area on your skin that you cannot account for, one that feels slightly firm or waxy, or that has slowly appeared without a prior wound, it warrants assessment.
When in Doubt, Get It Checked
None of these comparisons are a substitute for a clinical examination. Basal cell carcinoma can present in multiple ways depending on its subtype, location, and the individual’s skin tone, which is why even experienced clinicians use dermoscopy to assess lesions accurately. If a lesion is new, changing, bleeding, or simply not healing, the safest course of action is always to have it evaluated by a dermatologist.
How to Prevent Basal Cell Carcinoma
Because basal cell carcinoma is primarily driven by cumulative UV exposure, the majority of cases are preventable with consistent sun protection habits over time. Prevention is particularly important for those who have already had a BCC diagnosis, as having one significantly increases the likelihood of developing another.
Wear Sunscreen Daily
Daily broad-spectrum SPF 30 or higher is the single most important preventative measure against BCC and skin cancer more broadly. UV damage accumulates over a lifetime, not just from to beach holidays or sunny days. Incidental exposure during daily activities, driving, and time near windows contributes meaningfully to cumulative UV load. Applying sunscreen every morning, year-round, is the most effective habit you can build.
Some of Dr Derrick Phillips’ favorite sunscreens are:
- Eucerin Sun Gel-Cream Oil Control SPF 50+
- Anthelios UVMune 400 Invisible Fluid Spf50+ Sun Cream
- Avene SPF 50+ Cream
- Heliocare 360 Water-gel SPF50
Learn more about chemical vs mineral sunscreen here.
Cover Up in the Sun
Sunscreen alone is not always sufficient, particularly during prolonged outdoor exposure. Wide-brimmed hats, UV-protective clothing, and sunglasses provide physical protection for areas that are frequently missed or where sunscreen wears off — the nose, ears, scalp, and the back of the neck, which are among the most common sites for BCC.
Dr Derrick Phillips breaks down UV Clothing Protection here and more sun protection tips in this inews feature.
Avoid Tanning Beds
Tanning beds expose the skin to concentrated UV radiation and are a well-established risk factor for all forms of skin cancer, including basal cell carcinoma. There is no safe level of tanning bed use.
Seek Shade During Peak Hours
UV radiation is strongest between 11am and 3pm. Seeking shade, wearing protective clothing, and reducing direct sun exposure during these hours, particularly in summer and in high-altitude or high-UV environments, meaningfully reduces cumulative UV damage over time.
Have Your Skin Checked Regularly
Preventative skin checks with a dermatologist allow suspicious lesions to be identified and treated at the earliest possible stage, before they require complex intervention. This is particularly important for those with a personal or family history of skin cancer, fair skin, a history of significant sun exposure, or a large number of moles. An annual skin check is a straightforward step that can make a significant difference in outcomes.
Common Questions We Answer in Clinic About Basal Cell Skin Cancer
Can basal cell carcinoma spread to other organs?
Basal cell carcinoma very rarely metastasises, which is what makes it distinct from more aggressive skin cancers like melanoma. However, this does not mean it is harmless. Left untreated, BCC can grow into surrounding tissue, cartilage, bone, and nerves — particularly on the face — making early treatment significantly less complex than delayed intervention.
How fast does basal cell carcinoma grow?
BCC typically grows slowly over months or years, which is one of the reasons early signs are frequently overlooked. The rate of growth varies by subtype — nodular BCC tends to grow more slowly, while morphoeic BCC can be more infiltrative and harder to detect. Slow growth does not mean it is safe to monitor without a clinical assessment.
Can basal cell carcinoma be mistaken for something else?
Yes, and this is one of the most common reasons diagnosis is delayed. On the face, BCC is frequently confused with a persistent pimple, or patch of dry skin. Elsewhere on the body it can resemble eczema, a scar, or in darker skin tones, a mole or melanoma. If a lesion does not behave the way you would expect — particularly if it bleeds, fails to heal, or slowly enlarges — it should be examined.
What does basal cell carcinoma look like on the nose?
The nose is the single most commonly affected site for BCC. It typically presents as a pearly or shiny bump, sometimes with small visible blood vessels on the surface, or as a sore that repeatedly crusts and fails to heal. Because the nose has limited surrounding tissue, lesions in this area require prompt assessment. The deeper a lesion grows before treatment, the more complex the procedure required to remove it.
Is basal cell carcinoma treatment available on the NHS?
Yes. Basal cell carcinoma is treated on the NHS, typically via a referral from your GP following a suspicious lesion assessment. However, wait times for dermatology referrals can be lengthy. Patients who prefer faster access to diagnosis and treatment, or who want specialist dermatologist-led care, can be seen privately.
Schedule a consultation with Dr Derrick Phillips in one of his private dermatology pratices in London for a comprehensive mole and skin cancer check.
Is basal cell carcinoma curable?
When detected early, basal cell carcinoma is highly treatable and, in most cases, completely curable. The cure rate for early-stage BCC treated with surgical excision or Mohs micrographic surgery is over 95%. This is why early detection and prompt treatment are the most important factors in managing the condition successfully.
