Back acne, often referred to as bacne, is a common and sometimes persistent skin condition that can affect both teenagers and adults. For many, back acne is more than just a breakout. It can impact confidence, make you second-guess what you wear, and leave you feeling frustrated when nothing seems to work.
Back acne can be more difficult to treat than facial acne because the skin on the back is thicker and produces more oil, which can make it more prone to breakouts.
For patients seeking back acne treatment, effective management requires a targeted approach that addresses the underlying mechanisms, such as excess sebum production, follicular blockage, bacterial proliferation, and inflammation.
Dr Derrick Phillips outlines 3 dermatologist-approved treatment steps to take control of your bacne for good.
What Causes Bacne?
Bacne develops in the same way as acne on the face, but is often made worse by environmental and mechanical factors.
It’s driven by a combination of processes within the skin:
- Increased oil (sebum) production, often influenced by hormones
- Build-up of dead skin cells, which clog the pores
- Overgrowth of acne-causing bacteria (Cutibacterium acnes)
- Inflammation within the hair follicle
These internal factors are often compounded by external triggers such as sweating, occlusion, and friction from tight clothing or backpacks, which can worsen breakouts on the back.
The back has a higher concentration of oil glands, and because it’s harder to reach and treat with topical products, breakouts in this area are often more persistent.
If your back acne isn’t responding to conventional treatments, particularly if you live in a hot or humid environment, it may be worth considering fungal acne as a possible cause. This article breaks down what that means.
How to Get Rid of Back Acne: Dermatologist-Recommended Approach
Effective bacne treatments typically involve a combination of topical and, where necessary, systemic therapies.
1. Benzoyl Peroxide Wash (5%)
A benzoyl peroxide wash is often recommended as a first-line treatment for inflammatory bacne.
This will:
- Reduces Cutibacterium acnes through antimicrobial activity
- Decreases inflammatory lesions
- Helps prevent new breakoutsb
Benzoyl peroxide is particularly effective for patients seeking to improve their bacne quickly, especially in the inflammatory stages.
2. Topical Retinoids
Topical retinoids are a key part of acne treatment and play an important role in long-term control.
They work by:
- Normalising skin cell turnover
- Preventing clogged pores
- Reducing inflammation
Retinoids are particularly helpful for treating comedonal acne and reducing the risk of recurrence. In more persistent cases, prescription-strength options such as Trifarotene may be needed.
3. Oral Antibiotics
For moderate to severe back acne, particularly when breakouts are inflamed or widespread, a course of oral antibiotics may be recommended.
They work by:
- Reducing the number of acne-causing bacteria
- Calming inflammation within the skin
These treatments are usually prescribed for a limited period and are combined with topical therapies to reduce the risk of antibiotic resistance and improve overall outcomes.
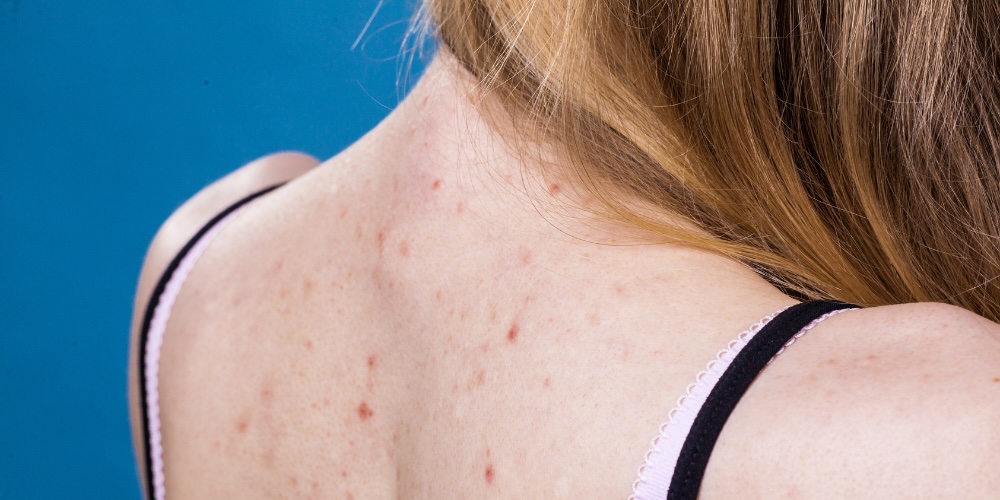
Lifestyle Changes to Improve Bacne
While medical treatment is central, simple day-to-day measures can help improve outcomes:
- Showering soon after sweating
- Wearing loose, breathable clothing
- Avoiding tight or occlusive fabrics
- Using non-comedogenic body care products
- Minimising friction and avoiding picking
Consistency is key, both with treatment and your skincare routine, as it can take 6-8 weeks to see a meaningful improvement.
When to See a Dermatologist
If acne is persistent, painful, widespread, or leaving marks, professional assessment is recommended to prevent long-term skin damage.
A dermatologist, like Dr Derrick Phillips, can tailor therapy, prescribe advanced treatments, and address underlying contributing factors, including hormonal influences where relevant.